Abstract
-
Purpose
- To evaluate the effects of the ratio of anterior chamber depth to axial length (ACD/AL), as well as axial length (AL) itself, on the accuracy of conventional intraocular lens (IOL) power calculation formulas in eyes with axial myopia.
-
Methods
- This retrospective cross-sectional study included 60 eyes from 44 patients with an AL greater than 25.0 mm who underwent uncomplicated phacoemulsification with IOL implantation. Eyes were categorized into high and low AL groups using an AL threshold of 27.0 mm, and into high and low ACD/AL groups based on the median ACD/AL value of 13.4. The median absolute errors (MedAEs) predicted by the Sanders-Retzlaff-Kraff theoretical (SRK/T) and Haigis formulas were compared according to AL and ACD/AL groupings.
-
Results
- In the low ACD/AL group and in the high AL group, the MedAEs predicted by the Haigis formula were lower than those predicted by the SRK/T formula (P=0.002 and P=0.012, respectively). The MedAEs predicted by both the SRK/T and Haigis formulas were significantly lower in the high ACD/AL group than in the low ACD/AL group (P<0.001 and P=0.010, respectively). In contrast, no significant difference was observed between the low and high AL groups in the MedAEs predicted by the Haigis formula. When the ACD/AL ratio was less than 13.4, postoperative refractive outcomes were more hyperopic with both formulas.
-
Conclusion
- In eyes with a long AL and a relatively shallow ACD, the Haigis formula demonstrated superior accuracy among conventional IOL power calculation formulas. Under these anatomical conditions, targeting slightly more myopic postoperative refractions may therefore be advisable.
-
Keywords: Intraocular lens; Anterior chamber depth; Axial length; Axial myopia
Introduction
Phacoemulsification with intraocular lens (IOL) implantation is one of the most widely performed surgeries by ophthalmologists, and refractive outcomes after cataract surgery have greatly improved over time [1-3]. IOL power calculation is important for attaining optimal refractive outcomes. Axial length (AL) measurement (54%) is the most common source of miscalculation with ultrasound biometry, followed by postoperative anterior chamber depth (ACD) estimation (38%), and corneal power (K) measurement (8%) [4]. Due to the availability of more accurate AL measurements by optical biometry using the IOLMaster (Carl Zeiss Meditec), the error contribution from AL measurements has decreased [5-8] and was found to be less than the error contribution from ACD prediction [3].
Long axial myopic eyes have a high risk for unexpected postoperative refractive effects after cataract surgery with IOL implantation [9-15]. In recent studies, the Haigis formula was reported to have the lowest refractive error in eyes with a long AL, followed by the Sanders-Retzlaff-Kraff theoretical (SRK/T) formula [10,16]. The Haigis formula, which is a fourth-generation formula, may be the most accurate because the postoperative effective lens position (ELP) is calculated using the measured ACD, whereas, in the SRK/T formula, ELP is estimated from the AL, K, and A constants using the corneal height formula [16,17]. The SRK/T formula assumes that eyes with a long AL will have deeper ACD than eyes with a short AL. In other words, according to the SRK/T formula, the estimated ELP is expected to increase as AL increases. Thus, when eyes with a long AL have a shallow ACD, the estimated ELP tends to be deeper than the actual ELP, resulting in myopic refractive outcomes. Therefore, we hypothesized that the accuracy of the SRK/T formula in eyes with long AL may be influenced by the ratio of ACD to AL (ACD/AL).
The aim of this study was to evaluate the effects of ACD/AL and AL on the accuracy of IOL power calculations made using the IOLMaster 500 by the SRK/T and Haigis formulas in eyes with a long AL of more than 25.0 mm.
Methods
Ethics statement
This retrospective study was approved by the Institutional Review Board of the Korea University Guro Hospital (IRB No. 2012GR0192). The requirement for informed consent was waived due to the retrospective nature of the study and the use of deidentified data. The study was conducted in accordance with the tenets of the Declaration of Helsinki.
Patient and study design
This retrospective study included 60 eyes from 44 patients who underwent uncomplicated phacoemulsification with Acrysof IQ (SN60WF, Alcon; 23 eyes from 19 patients), Rayner Superflex 620H (Rayner Intraocular Lenses Limited; 12 eyes from 10 patients), Tecnis ZCB00 1 piece (Abbott Medical Optics Inc.; 12 eyes from nine patients), Hoya NY-60 (HOYA Corp.; seven eyes from seven patients), or Sensar AR40E (6 eyes from four patients) IOL implantation at our institute between September 2009 and January 2012. Eyes with AL measurements of more than 25.0 mm as made by the IOLMaster 500 and with at least three valid measurements with a signal to noise ratio (SNR) above 1.5 for a single measurement and a SNR above 2.0 for the composite signal were included. Patients who had best-corrected visual acuities (BCVA) of less than 20/40 in the operated eye after cataract surgery, traumatic cataracts, previous ocular surgeries such as penetrating keratoplasty or refractive surgery, surgery complications such as anterior or posterior capsular ruptures, sulcus fixated lenses, IOL exchanges, postoperative complications, or prior retinal detachments were excluded.
Preoperative K, AL, and ACD were measured using the IOLMaster 500 ver. 5.02. All measurements were taken by a single trained ophthalmic examiner. IOL power was calculated using the SRK II, SRK/T, Holladay 1, Hoffer Q, and Haigis formulas. The IOL constants for all IOLs were obtained from the User Group for Laser Interference Biometry database [18]. Postoperative uncorrected visual acuity, manifest refraction, and BCVA were measured three to 10 weeks after the operation.
All phacoemulsification and IOL implantations were performed by one of two surgeons (YYK, JSS) at our institute. After topical anesthesia with Alcaine (proparacaine hydrochloride 0.5%), a 2.2- or 2.75-mm temporal clear corneal incision was made and a continuous curvilinear capsulorrhexis slightly smaller than the IOL optic size was created with a 26-gauge needle. A standard phacoemulsification technique was used and the IOL was inserted into the capsular bag using an injector system.
Median absolute error (MedAE) was defined as the median absolute value of the predicted refractive error. The predicted refractive error was defined as the difference between the observed refractive spherical equivalent at postoperative 3 weeks and the preoperative refraction predicted by the IOLMaster 500 for the implanted IOL using the SRK II, SRK/T, Holladay 1, Hoffer Q, and Haigis formulas (predicted refractive error=postoperative spherical equivalent-preoperative predicted refraction). ACD/AL was defined as the actual measured ACD divided by AL multiplied by 100. To evaluate the effects of ACD/AL and AL on the accuracy of IOL power calculation in eyes with a long AL, the sample eyes were divided into high AL group and low AL group based on AL of 27.0 mm, and into a high ACD/AL group and low ACD/AL group by the median ACD/AL value (13.4).
Theoretical investigation of the SRK/T and Haigis formulas
The SRK/T formula uses AL and K to estimate ELP using a corneal height calculation formula. Corneal height calculations using the IOL power calculation algorithm of the SRK/T formula are as follows [17,19,20]:
1. Corneal radius of curvature, r=337.5K
2. Corrected AL, LCOR:
If L ≤ 24.2, then LCOR=L
If L > 24.2, then LCOR=L-3.446+1.716L-0.0237L2
3. Computed corneal width, Cw:
Cw=-5.40948+0.58412 LCOR+0.098 K
4. Corneal height, H, calculation:
H=r-r2-Cw/22
If r2-Cw/22<0, then r2-Cw/22=0
Where r is the corneal radius, K is corneal power, and L is AL.
The Haigis formula [21] uses the following regression equation for ELP prediction:
ELP=a0+a1×ACD+a2×AL
Where a0 is a constant related to the ACD constant, a1 is the regression coefficient for preoperative ACD, and a2 is the regression coefficient for preoperative AL. The mean a2 constant of the Haigis formula used in this study was 0.218.
Statistical analysis
Statistical analyses were performed using repeated measures ANOVA, Mann-Whitney test, and Wilcoxon’s signed rank test using SPSS ver. 12.0 (IBM Corp.). Results were considered statistically significant if the P-value was <0.05.
Results
Sixty eyes from 44 patients that underwent phacoemulsification with IOL implantation were included in the present study. The mean age of subjects was 59.6±13.5 years (range, 16–83 years). Sixteen patients were male (36.4%) and 28 patients were female (63.6%). The mean AL was 27.76±2.51 mm. The laterality, K, and calculated IOL power are shown in Table 1.
The calculated MedAEs by the SRK II, SRK/T, Holladay 1, Hoffer Q, and Haigis formulas are shown in Table 2. According to repeated measures ANOVA, the MedAE predicted by the Haigis formula (0.39 diopter [D]) was significantly smaller than that predicted by the SRK II (1.13 D), Holladay 1 (0.46 D), and Hoffer Q formulas (0.53 D; P<0.001, P<0.001, and P<0.001, respectively). However, the difference between the MedAEs predicted by the SRK/T formula (0.39 D) and the Haigis formula (0.39 D) was not statistically significant.
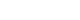
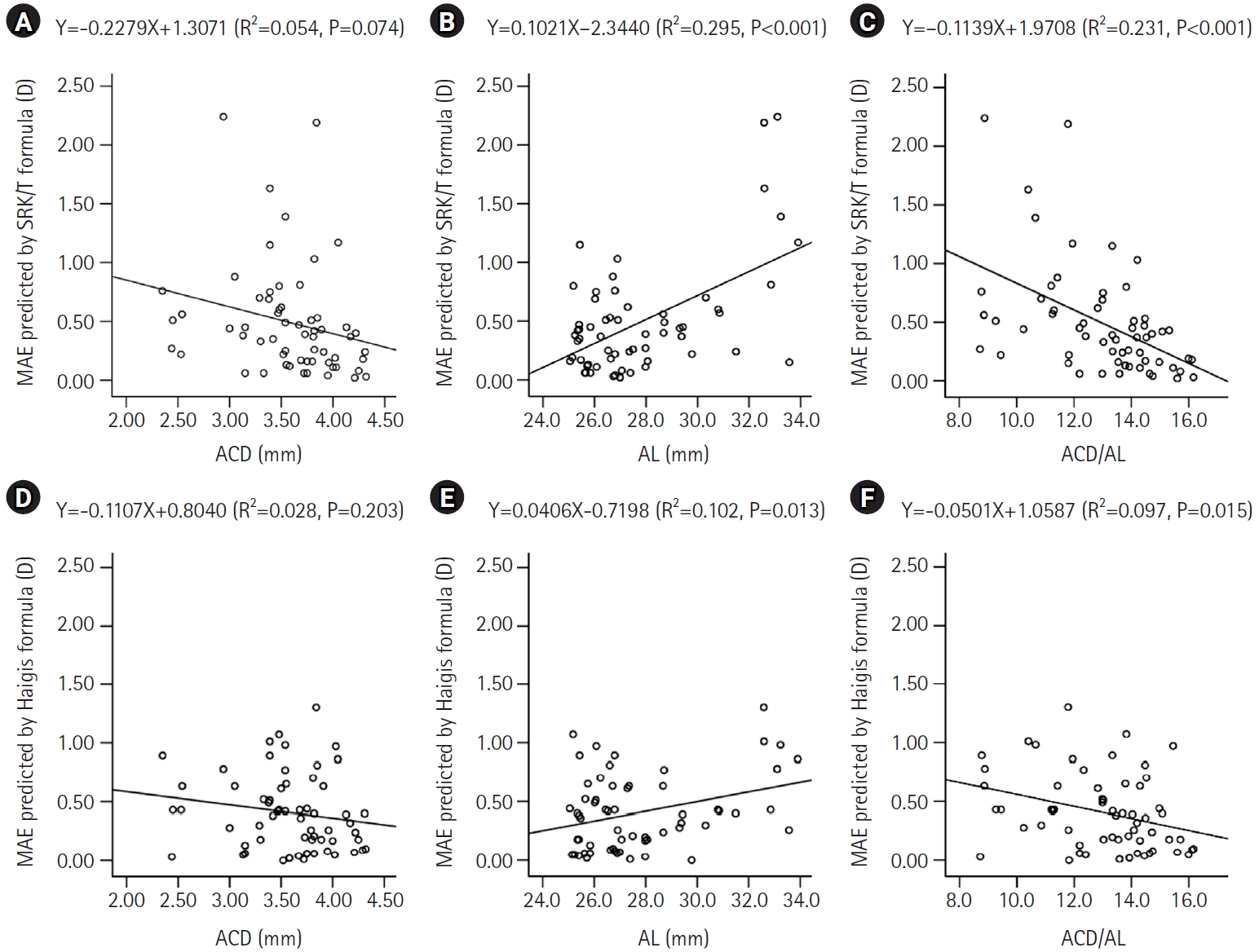
Fig. 1 shows the linear regression analysis of the relationship between the ACD, AL, ACD/AL, and the absolute value of the predicted refractive error by the SRK/T and Haigis formulas. The absolute value of the predicted refractive error by the SRK/T and Haigis formulas both decrease as ACD and ACD/AL increase and as AL decreases. AL and ACD/AL are significantly correlated with the absolute value of the predicted refractive error by the SRK/T formula (R2=0.295, P<0.001 and R2=0.231, P<0.001, respectively) and the Haigis formula (R2=0.102, P=0.013 and R2=0.097, P=0.015, respectively).
Table 3 shows the MedAEs predicted by the SRK/T and Haigis formulas according to ACD/AL and AL. In the low ACD/AL group and the high AL group, the Haigis formula (0.43 and 0.39 D, respectively) was more accurate than the SRK/T formula (0.59 and 0.49 D, respectively; P=0.002 and P=0.012, respectively). There were no significant differences between the MedAEs predicted by the SRK/T and Haigis formulas for the high ACD/AL group and the low AL group. The SRK/T and Haigis formulas were more accurate for the high ACD/AL group (0.22 and 0.23 D, respectively) than for the low ACD/AL group (0.59 and 0.43 D, respectively; P<0.001 and P=0.010, respectively). The SRK/T formula was more accurate for the low AL group (0.35 D) than for the high AL group (0.49 D, P=0.039). However, there was no significant difference in the MedAEs predicted by the Haigis formula between the low AL group and the high AL group.
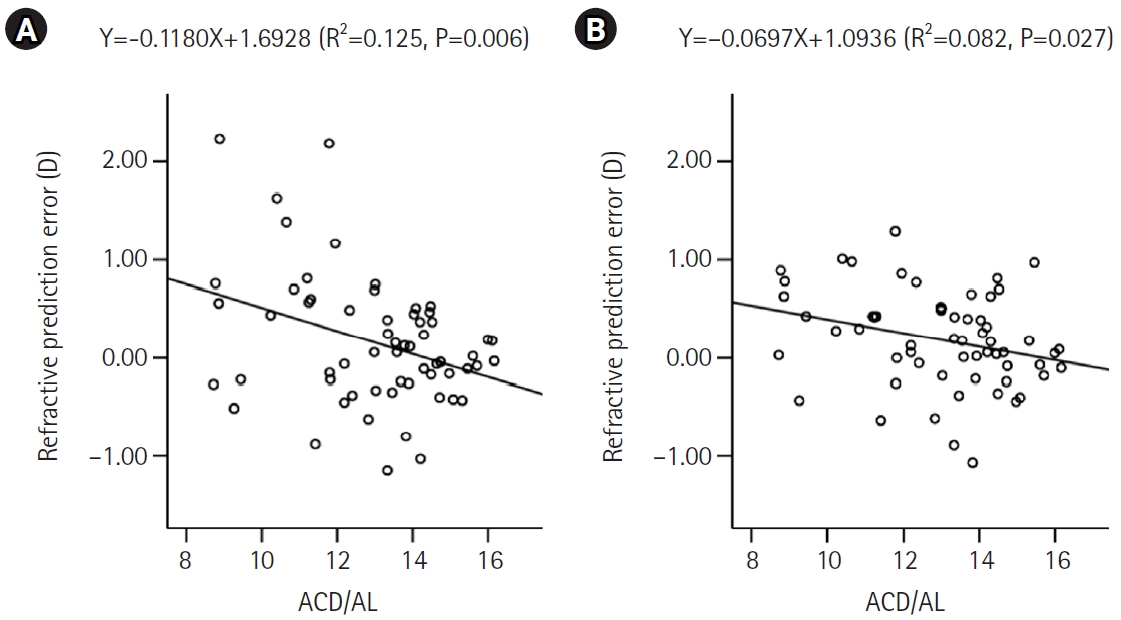
There was a significant negative correlation between the ACD/AL and the predicted refractive error by the SRK/T and Haigis formulas (Fig. 2). When the ACD/AL was smaller than 13.4, the refractive outcome was more hyperopic.
Theoretical investigation of the SRK/T and Haigis formulas
When the estimated corneal height H (SRK/T step 4) was set as the preoperative ACD, the calculation of the theoretical ACD/AL in the SRK/T formula is as follows:
Theoretical ACD/AL = r-r2-Cw/22AL
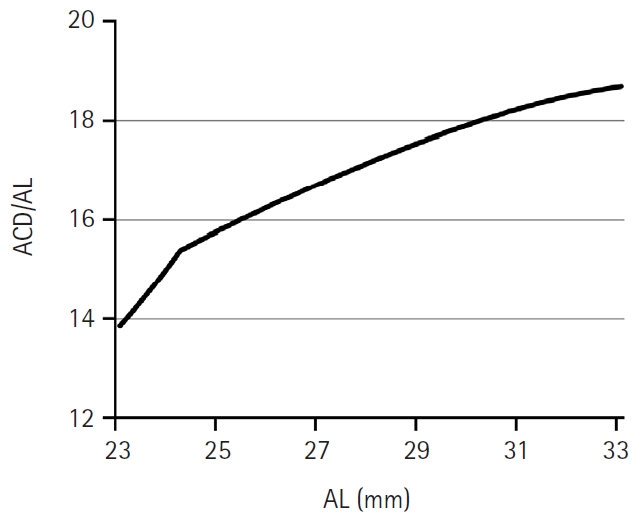
Fig. 3 shows the theoretical ACD/AL with varying AL after K was set to 44.4 D (the mean K of this study). The theoretical values of ACD/AL increase as AL increases in the SRK/T formula.
According to the regression equation of the ELP prediction of the Haigis formula, when ACD was set to 3.58 (the study mean), the difference of ELP between eyes with an AL of 23.39 mm (the mean AL in the Haigis formula) and eyes with an AL of 27.8 mm (this study’s mean) was calculated to be 0.97 mm.
Discussion
The possible sources of postoperative refractive error in eyes with long AL include inaccurate measurement of AL [22], especially in eyes with posterior pole staphyloma [11], and the implantation of minus IOLs [9,23,24]. IOLMaster 500 yielded significantly better IOL power predictions and AL measurements in cataract surgery than ultrasonic biometry did [2,25]. Previous studies have shown that in cases of eyes with staphyloma, AL measurement by IOLMaster 500 was more accurate than by ultrasonic biometry [19]. Accurate ACD prediction has become increasingly important at the accuracy of IOL power prediction, as the error contribution from AL measurements has decreased [3,5-8].
Previous studies have shown that the Haigis formula was more accurate than several third-generation formulas at IOL power prediction in eyes with a long AL [10,16]. Bang et al. [16] analyzed 53 eyes with an AL of more than 27 mm that underwent uncomplicated cataract surgeries. They categorized the eyes into three subgroups by AL and reported that the SRK/T formula was most accurate in eyes with an AL of 27 to 29.07 mm, whereas the Haigis formula was most accurate in eyes with an AL of more than 29.07 mm. Wang et al. [10] analyzed 68 eyes with an AL of more than 25 mm and showed that the Haigis and SRK/T formulas were most accurate at IOL power prediction in eyes with an AL between 25.0 to 28.0 mm. However, the SRK/T formula was less accurate than the Haigis formula in eyes with an AL of longer than 28.0 mm. In the present study, the Haigis and SRK/T formulas were found to be the most accurate in terms of refractive error in eyes with an AL of more than 25 mm, and there was no statistically significant difference between the Haigis formula and the SRK/T formula in eyes with an AL between 25.0 to 26.99 mm. However, the Haigis formula was more accurate than the SRK/T formula in eyes with an AL of longer than 27.0 mm. These findings were similar to those reported by previous studies [10,16].
Previous studies have analyzed the accuracy of IOL formulas according to AL in eyes with a long AL. However, in the present study, we evaluated the accuracy of the IOL formulas not only according to AL, but also according to ACD/AL. The Haigis formula, a fourth-generation formula, uses the actual measured ACD to estimate ELP. However, third-generation formulas such as the SRK/T, Holladay 1, and Hoffer Q formulas do not use the actual measured ACD, but instead determine ELP using AL and K [3,16,17,20]. Therefore, the error from estimating the ELP should be taken into consideration when evaluating the accuracy of IOL formulas in long eyes.
In the present study, we hypothesized that the accuracy of IOL formulas in eyes with a long AL may be influenced by ACD/AL. We evaluated the effects of ACD/AL and AL on the accuracy of IOL power calculations made using the IOLMaster 500. The MedAE predicted by the SRK/T formula was found to be more accurate in the high ACD/AL group than in the low ACD/AL group. The reason for this result is that, in the SRK/T formula, estimated ACD/AL increases as AL increases, as shown in Fig. 3. This means that the increase in ACD is assumed to be greater than that of AL. Thus, MedAE predicted by the SRK/T formula is more accurate in long eyes with high ACD/AL than with low ACD/AL. The MedAE predicted by the Haigis formula was also found to be more accurate in the high ACD/AL group than in the low ACD/AL group. Although the Haigis formula uses the actual measured preoperative ACD in ELP prediction, the ELP prediction is affected by ACD/AL because ELP prediction made using the Haigis formula includes both ACD and AL. Olsen [3] showed that the corresponding refractive error in an eye with an AL of 28.0 mm was about 0.2 D, with a 0.25 mm error in ELP prediction. Thus, the corresponding refractive error from a 0.97 mm difference in ELP prediction between eyes with an AL of 23.39 mm (the mean AL in the Haigis formula) and eyes with an AL of 27.85 mm (this study’s mean) will be higher than 0.2 D, and ACD/AL does affect the refractive error as calculated by the Haigis formula.
Olsen [3] showed that the refractive error of ELP prediction is strongly dependent on AL and that accurate prediction of ELP is more important in short eyes than in long eyes. Although postoperative ACD is more important in short eyes than in long eyes [26], ACD/AL should be taken into consideration when evaluating the accuracy of IOL formulas when used with long eyes. In the present study, the MedAE predicted by the SRK/T and Haigis formulas were found to be less accurate and refractive outcomes were more hyperopic in the low ACD/AL group. Haigis formula was especially more affected by ACD/AL than by AL. Therefore, IOLs with more myopic targets are recommended for eyes with a long AL and a relatively small ACD/AL.
There are several limitations to the present study. First, the sample size was relatively small, and the medical records were reviewed retrospectively. Second, multiple IOL models were implanted. Consequently, the number of eyes for each IOL model was insufficient to allow a robust subgroup analysis of the effects of different IOL designs on refractive outcomes. However, implanting different IOLs in axial myopia cannot be avoided, as the range of the IOL power according to the IOL type is different.
In conclusion, the SRK/T formula was similarly accurate in IOL power prediction in long eyes with high ACD/AL. However, in patients with a long AL and a relatively small ACD, the Haigis formula would be the better choice for calculating the IOL power. Besides, IOLs with more myopic targets are recommended for eyes with a low ACD/AL than with a high ACD/AL in the SRK/T and Haigis formulas.
Article Information
Author contributions
Conceptualization: YE, JSS. Formal analysis: all authors. Investigation: all authors. Methodology: YE, DHK, JSS. Supervision: YE, JSS. Writing – original draft: YE. Writing – review & editing: all authors. Final approval of the manuscript: all authors.
Conflicts of interest
No potential conflict of interest relevant to this article was reported.
Funding
None.
Acknowledgments
We sincerely thank Dr. Yong Yeon Kim (Kim’s Eye Hospital, Seoul, Korea) for performing cataract surgeries and contributing to the clinical care of the patients whose medical records were used in this retrospective study.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Fig. 1.Linear regression analysis illustrating the relationships among anterior chamber depth (ACD), axial length (AL), the ACD to AL ratio (ACD/AL), and the absolute value of the predicted refractive error calculated using the Sanders-Retzlaff-Kraff theoretical (SRK/T) and Haigis formulas. Panels A–C present the associations for the SRK/T formula with ACD (A), AL (B), and ACD/AL (C), whereas panels D–F depict the corresponding associations for the Haigis formula with ACD (D), AL (E), and ACD/AL (F). MAE, mean absolute error; D, diopters.
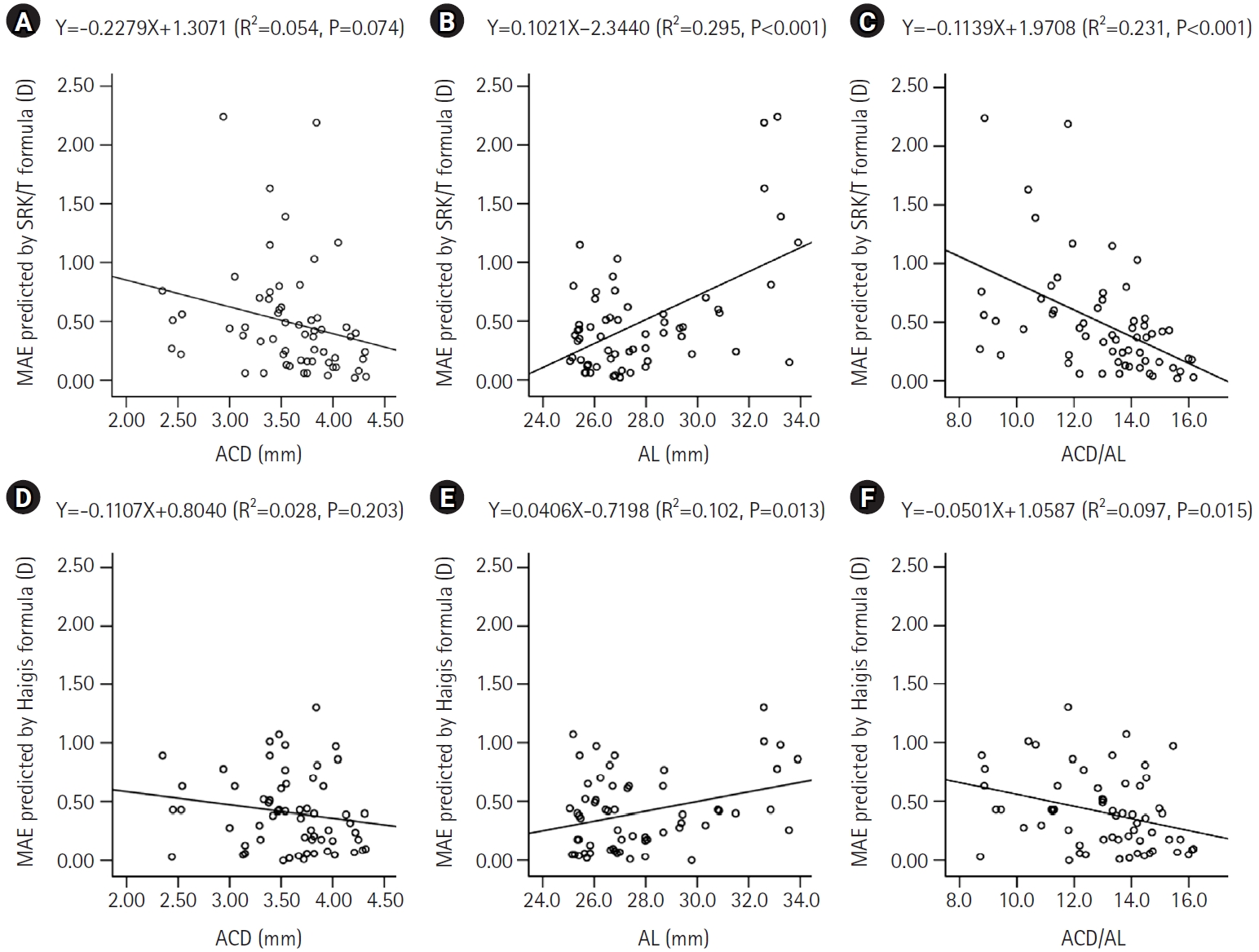
Fig. 2.Comparison of the predicted refractive error according to the anterior chamber depth to axial length ratio (ACD/AL) using the Sanders-Retzlaff-Kraff theoretical formula (A) and the Haigis formula (B). D, diopters.
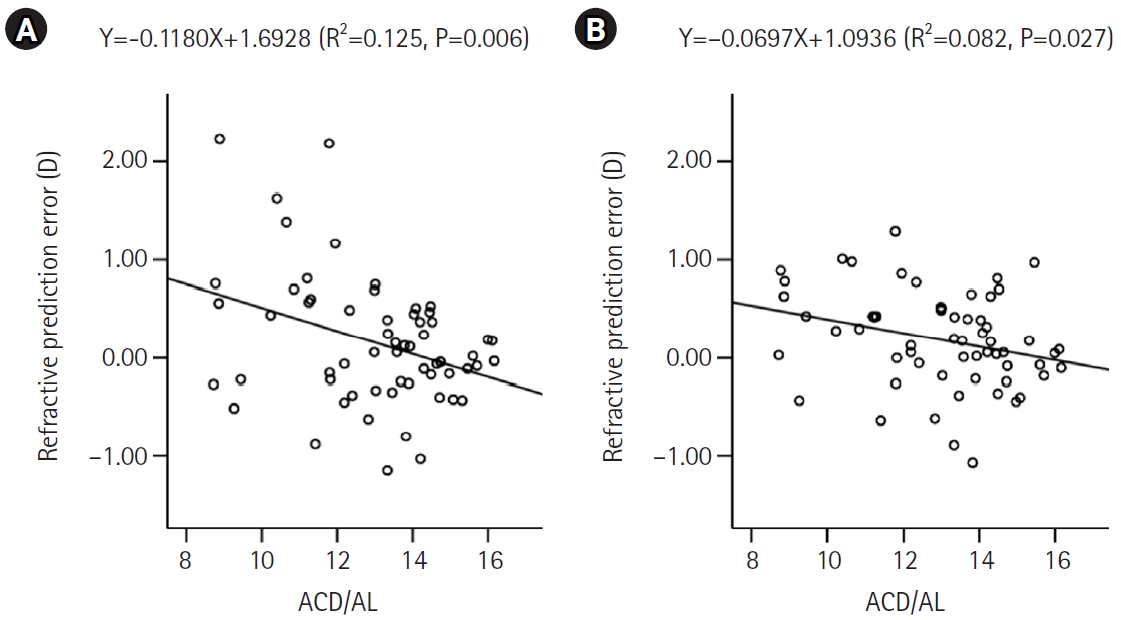
Fig. 3.Graph depicting the theoretical ratio of ACD/AL across varying AL, generated after setting the corneal power to 44.4 diopters, corresponding to the mean corneal power in this study, using the Sanders-Retzlaff-Kraff theoretical formula. ACD/AL, anterior chamber depth to axial length ratio.
Table 1.The clinical and demographic characteristics of the subjects included in the present study (n=60)
|
Demographic |
Value |
|
Age (yr) |
59.6±13.5 (16–83) |
|
Sexa)
|
|
|
Male |
16 (36.4) |
|
Female |
28 (63.6) |
|
Lateralitya)
|
|
|
Right eye |
34 (56.7) |
|
Left eye |
26 (43.3) |
|
Corneal power (D) |
44.43±1.50 (41.57 to 48.49) |
|
Anterior chamber depth (mm) |
3.58±0.48 (2.35 to 4.32) |
|
Axial length (mm) |
27.76±2.51 (25.05 to 33.90) |
|
IOL power (D) |
9.2±6.7 (–7.0 to 18.0) |
Table 2.MedAE and MAE as predicted by different formulas
|
Formula |
Whole subjects (n=60) |
P-valuea)
|
|
MedAE (D) |
MAE (D) |
Range (D) |
|
SRK II |
1.13 |
1.22 |
0.02–4.28 |
<0.001 |
|
SRK/T |
0.39 |
0.49 |
0.02–2.24 |
0.077 |
|
Holladay 1 |
0.46 |
0.61 |
0.02–1.99 |
<0.001 |
|
Hoffer Q |
0.53 |
0.71 |
0.00–2.45 |
<0.001 |
|
Haigis |
0.39 |
0.41 |
0.00–1.30 |
- |
Table 3.MedAE and MAE as predicted by the SRK/T and Haigis formulas according to the ACD/AL and AL
|
Formula |
Low ACD/AL (n=30) |
High ACD/AL (n=30) |
P-valuea)
|
Low AL (n=33) |
High AL (n=27) |
P-valueb)
|
|
MedAE (D) |
MAE (D) |
MedAE (D) |
MAE (D) |
MedAE (D) |
MAE (D) |
MedAE (D) |
MAE (D) |
|
SRK/T |
0.59 |
0.70 |
0.22 |
0.28 |
<0.001 |
0.35 |
0.38 |
0.49 |
0.63 |
0.039 |
|
Haigis |
0.43 |
0.50 |
0.23 |
0.32 |
0.010 |
0.38 |
0.38 |
0.39 |
0.45 |
0.250 |
|
P-valuec)
|
0.002 |
0.449 |
|
0.948 |
0.012 |
|
References
- 1. Mamalis N. Intraocular lens power accuracy: how are we doing? J Cataract Refract Surg 2003;29:1‒3. ArticlePubMed
- 2. Olsen T. Improved accuracy of intraocular lens power calculation with the Zeiss IOLMaster. Acta Ophthalmol Scand 2007;85:84‒7. ArticlePubMed
- 3. Olsen T. Calculation of intraocular lens power: a review. Acta Ophthalmol Scand 2007;85:472‒85. ArticlePubMed
- 4. Olsen T. Sources of error in intraocular lens power calculation. J Cataract Refract Surg 1992;18:125‒9. ArticlePubMed
- 5. Olsen T, Thorwest M. Calibration of axial length measurements with the Zeiss IOLMaster. J Cataract Refract Surg 2005;31:1345‒50. ArticlePubMed
- 6. Findl O, Kriechbaum K, Sacu S, et al. Influence of operator experience on the performance of ultrasound biometry compared to optical biometry before cataract surgery. J Cataract Refract Surg 2003;29:1950‒5. ArticlePubMed
- 7. Kielhorn I, Rajan MS, Tesha PM, et al. Clinical assessment of the Zeiss IOLMaster. J Cataract Refract Surg 2003;29:518‒22. ArticlePubMed
- 8. Connors R, Boseman P, Olson RJ. Accuracy and reproducibility of biometry using partial coherence interferometry. J Cataract Refract Surg 2002;28:235‒8. ArticlePubMed
- 9. Tsang CS, Chong GS, Yiu EP, Ho CK. Intraocular lens power calculation formulas in Chinese eyes with high axial myopia. J Cataract Refract Surg 2003;29:1358‒64. ArticlePubMed
- 10. Wang JK, Hu CY, Chang SW. Intraocular lens power calculation using the IOLMaster and various formulas in eyes with long axial length. J Cataract Refract Surg 2008;34:262‒7. ArticlePubMed
- 11. Zaldivar R, Shultz MC, Davidorf JM, Holladay JT. Intraocular lens power calculations in patients with extreme myopia. J Cataract Refract Surg 2000;26:668‒74. ArticlePubMed
- 12. MacLaren RE, Sagoo MS, Restori M, Allan BD. Biometry accuracy using zero- and negative-powered intraocular lenses. J Cataract Refract Surg 2005;31:280‒90. ArticlePubMed
- 13. Drews RC. Results in patients with high and low power intraocular lenses. J Cataract Refract Surg 1986;12:154‒7. ArticlePubMed
- 14. Huber C. Effectiveness of intraocular lens calculation in high ametropia. J Cataract Refract Surg 1989;15:667‒72. ArticlePubMed
- 15. Kohnen S, Brauweiler P. First results of cataract surgery and implantation of negative power intraocular lenses in highly myopic eyes. J Cataract Refract Surg 1996;22:416‒20. ArticlePubMed
- 16. Bang S, Edell E, Yu Q, et al. Accuracy of intraocular lens calculations using the IOLMaster in eyes with long axial length and a comparison of various formulas. Ophthalmology 2011;118:503‒6. ArticlePubMed
- 17. Retzlaff JA, Sanders DR, Kraff MC. Development of the SRK/T intraocular lens implant power calculation formula. J Cataract Refract Surg 1990;16:333‒40. ArticlePubMed
- 18. User Group for Laser Interference Biometry (ULIB). Optimized IOL constants for the Zeiss IOLMaster calculated from patient data on file [Internet]. ULIB; c2016 [cited 2026 Jan 12]. Available from: http://ocusoft.de/ulib/c1.htm
- 19. Sheard RM, Smith GT, Cooke DL. Improving the prediction accuracy of the SRK/T formula: the T2 formula. J Cataract Refract Surg 2010;36:1829‒34. ArticlePubMed
- 20. Haigis W. Occurrence of erroneous anterior chamber depth in the SRK/T formula. J Cataract Refract Surg 1993;19:442‒6. ArticlePubMed
- 21. Haigis W. The Haigis formula. In: Shammas HJ, editor. Intraocular lens power calculations. Slack Inc.; 2004. p. 41‒57.
- 22. Kora Y, Koike M, Suzuki Y, et al. Errors in IOL power calculations for axial high myopia. Ophthalmic Surg 1991;22:78‒81. ArticlePubMed
- 23. Haigis W. Intraocular lens calculation in extreme myopia. J Cataract Refract Surg 2009;35:906‒11. ArticlePubMed
- 24. Petermeier K, Gekeler F, Messias A, et al. Intraocular lens power calculation and optimized constants for highly myopic eyes. J Cataract Refract Surg 2009;35:1575‒81. ArticlePubMed
- 25. Rajan MS, Keilhorn I, Bell JA. Partial coherence laser interferometry vs conventional ultrasound biometry in intraocular lens power calculations. Eye (Lond) 2002;16:552‒6. ArticlePubMedPDF
- 26. Eom Y, Kang SY, Song JS, et al. Comparison of Hoffer Q and Haigis formulae for intraocular lens power calculation according to the anterior chamber depth in short eyes. Am J Ophthalmol 2014;157:818‒24. ArticlePubMed
Citations
Citations to this article as recorded by

 , Jinhwan Park2
, Jinhwan Park2 , Youngbin Song2
, Youngbin Song2 , Dong Hyun Kim1
, Dong Hyun Kim1 , Jong Suk Song1
, Jong Suk Song1





 KSCRS
KSCRS
 ePub Link
ePub Link Cite
Cite